Whether you are eligibility for lower costs in the Marketplace and for Medicaid and CHIP is based on your modified adjusted gross income (your adjusted gross income plus any tax-exempt Social Security, interest, or foreign income you have).
Modified Adjusted Gross Income (MAGI): Three Step Evaluation Process
STEP ONE: Identify members of the applicant’s family who are part of the household.
STEP TWO: Add the income of relevant household members, applying the relevant income modifications.
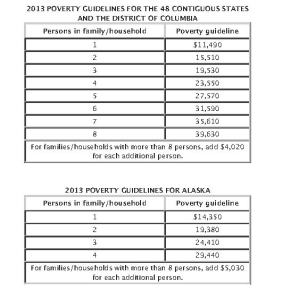
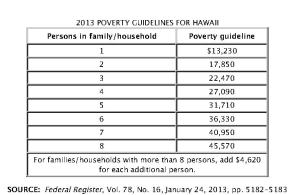
STEP THREE: Compare total household income to the Federal Poverty Level (FPL) for the number of people in their household.
Once you have determined your MAGI compare that income to the above tables to determine if your income qualifies you for the following:
- Expanded Medicaid – 138 percent of the federal poverty line;
- Premium assistance (or tax credits) – People can elect to take the credit on an “advance” basis if they need immediate help with their premium costs, or they can receive the credit when they file their income taxes. To qualify, people generally must have income between 100% and 400% of the federal poverty line and meet a range of non-financial criteria, including a requirement that they lack access to other affordable insurance options.
- Cost Sharing Reduction – After payment of premium and plan enrollment, cost-sharing reductions (CSR) help people with their out-of-pocket costs like deductibles, coinsurance and copayments.
• Only available to people who enroll in a silver plan which are referred to as “Enhanced Silver Plans” when they include CSR.
• There are three levels of savings available to people who qualify for a CSR.
• The level of savings (or tier) for which a family qualifies is based on the family’s income.
• The issuers provide the extra help with out-of-pocket costs by offering a silver plan with higher actuarial value.
• The higher the actuarial value, the lower the deductibles, coinsurance, and/or copayments.